Scleral Buckle Surgery: Saving Vision from Retinal Detachment
Introduction: The Light Against the Darkness of Retinal Detachment
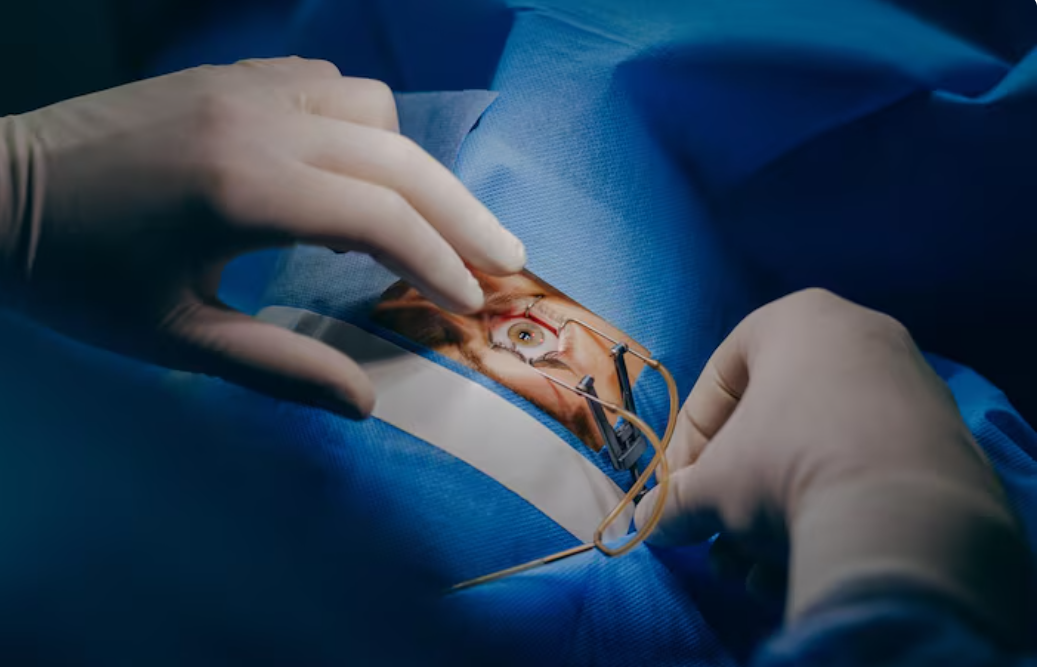
Retinal detachment. The very words can send shivers down the spine. Imagine the sudden, disconcerting experience of flashing lights, a shower of floaters obscuring your vision, or the sensation of a dark curtain gradually descending, blotting out the world around you. This is the terrifying reality of retinal detachment, a serious eye condition that demands immediate attention. Fortunately, a powerful and time-tested solution exists: scleral buckle surgery. Renowned for its high success rate, scleral buckle surgery stands as a stalwart defense against vision loss, an almost “indestructible” procedure in the eyes of many ophthalmologists. This article will delve into the intricacies of scleral buckle surgery, exploring what it is, how it works, what to expect, and ultimately, how it protects your precious eyesight.
Understanding Retinal Detachment: A Delicate Balance Disrupted
Before exploring the specifics of scleral buckle surgery, it’s crucial to understand the underlying problem: retinal detachment. The retina is a thin layer of light-sensitive tissue that lines the back of the eye, much like the film in a camera. It converts light into electrical signals that are sent to the brain, allowing us to see. Retinal detachment occurs when the retina separates from the underlying layer of blood vessels that provide it with oxygen and nourishment, called the choroid. This separation can occur due to various reasons, including:
* **Retinal Tears or Holes:** Small tears or holes can develop in the retina, allowing fluid from inside the eye to seep underneath, causing the retina to detach.
* **Tractional Detachment:** Scar tissue on the surface of the retina can contract, pulling the retina away from the back of the eye. This is often seen in people with diabetes.
* **Exudative Detachment:** Fluid can accumulate behind the retina without any tears or holes, pushing the retina away from the choroid. This can be caused by inflammatory conditions or tumors.
Scleral Buckle Surgery: The Principle of External Support
Scleral buckle surgery is an external procedure, meaning that the surgeon does not directly access the inside of the eye to repair the detachment. Instead, the procedure focuses on indenting the sclera, the white outer layer of the eye, to relieve traction on the retina and facilitate its reattachment. Think of it as gently pushing the wall of a room inward to meet a loose piece of wallpaper. The “buckle” itself is typically a small band made of silicone, sponge, or other biocompatible material.
The Surgical Procedure: A Step-by-Step Overview
The scleral buckle surgery is performed under general or local anesthesia, depending on the patient’s preference and the surgeon’s recommendation. The typical steps involved include:
1. **Exposure:** The surgeon carefully separates the conjunctiva (the clear membrane covering the white of the eye) to expose the sclera.
2. **Localization:** The retinal tears or holes are located using an indirect ophthalmoscope and indentation.
3. **Cryopexy or Laser Photocoagulation:** The surgeon uses cryopexy (freezing) or laser photocoagulation (burning) around the retinal tears or holes to create a scar that will seal the edges of the tear and prevent fluid from leaking underneath the retina.
4. **Scleral Buckle Placement:** The scleral buckle is then sutured to the sclera, indenting the eye wall and pushing it towards the detached retina. The buckle is positioned to provide support to the area of the retinal tear or detachment.
5. **Drainage of Subretinal Fluid (Optional):** In some cases, the surgeon may drain fluid from under the retina to help it flatten against the back of the eye. This step is not always necessary.
6. **Closure:** The conjunctiva is then stitched back into place.
Benefits of Scleral Buckle Surgery: A Legacy of Success
Scleral buckle surgery boasts a remarkable success rate in reattaching the retina, particularly for primary retinal detachments. It offers several key benefits:
* **High Success Rate:** As mentioned, scleral buckle surgery has a high success rate, often exceeding 80-90% for initial reattachment.
* **External Approach:** Being an external procedure, it avoids direct entry into the vitreous cavity (the gel-filled space inside the eye), minimizing the risk of certain complications.
* **Long-Term Stability:** The scleral buckle provides long-term support to the retina, reducing the risk of future detachments.
* **Versatility:** It can be used to treat a variety of retinal detachments, including those with multiple tears or detachments in the lower part of the eye.
Risks and Complications: Understanding the Potential Downsides
While scleral buckle surgery is generally safe and effective, like all surgical procedures, it carries certain risks and potential complications. These can include:
* **Infection:** Infection is a risk with any surgery, although it is rare.
* **Bleeding:** Bleeding during or after surgery is possible.
* **Double Vision:** The buckle can sometimes affect the muscles that control eye movement, leading to temporary or, rarely, permanent double vision.
* **Increased Eye Pressure (Glaucoma):** Scleral buckle surgery can sometimes increase the pressure inside the eye, leading to glaucoma.
* **Myopia (Nearsightedness):** The indentation of the sclera can sometimes cause a change in the shape of the eye, leading to increased nearsightedness.
* **Extrusion of the Buckle:** In rare cases, the buckle can erode through the conjunctiva and require removal.
* **Failure to Reattach the Retina:** While rare, the initial surgery may not be successful in reattaching the retina, requiring further intervention.
Recovery and Aftercare: What to Expect After Surgery
The recovery period following scleral buckle surgery typically involves several weeks. Patients can expect:
* **Eye Patch:** An eye patch will be worn for the first day or two to protect the eye.
* **Eye Drops:** Antibiotic and steroid eye drops will be prescribed to prevent infection and reduce inflammation.
* **Pain Management:** Pain medication may be needed for the first few days.
* **Activity Restrictions:** Avoid strenuous activities, heavy lifting, and bending over for several weeks.
* **Regular Follow-up Appointments:** Regular check-ups with the ophthalmologist are essential to monitor healing and ensure the retina remains attached.
* **Vision Improvement:** Vision improvement can be gradual and may take several weeks or months. The final visual outcome depends on the severity and duration of the detachment, as well as other individual factors.
Alternatives to Scleral Buckle Surgery: Exploring Other Options
While scleral buckle surgery remains a cornerstone of retinal detachment repair, other options are available, depending on the specific characteristics of the detachment. These include:
* **Pneumatic Retinopexy:** This involves injecting a gas bubble into the eye to push the retina back into place. It is typically used for simpler detachments with tears in the upper part of the eye.
* **Vitrectomy:** This procedure involves removing the vitreous gel from the eye and replacing it with saline solution or gas. It is often used for more complex detachments, such as those involving traction or bleeding.
Conclusion: Preserving Sight, One Buckle at a Time
Scleral buckle surgery stands as a testament to the ingenuity and effectiveness of modern ophthalmology. By providing external support and relieving traction on the retina, this procedure offers a high likelihood of successful reattachment and vision preservation. While it’s crucial to be aware of the potential risks and complications, the benefits of scleral buckle surgery often outweigh these concerns, especially when facing the daunting prospect of vision loss due to retinal detachment. Early detection and prompt intervention are key to maximizing the chances of a successful outcome and safeguarding your precious eyesight.
Frequently Asked Questions (FAQs)
- How long does scleral buckle surgery take?
- The surgery typically takes between 1 to 2 hours, but this can vary depending on the complexity of the case.
- Will I need to have the scleral buckle removed?
- In most cases, the scleral buckle remains in place permanently. Removal is only necessary in rare circumstances, such as infection or extrusion.
- When can I return to work after scleral buckle surgery?
- The return-to-work timeframe varies depending on the nature of your job. Generally, you can expect to return to work within 2 to 4 weeks, avoiding strenuous activities during this period.